Ο ιός των θηλωμάτων (Papilomma virus, PV) ανήκει σε μια μεγάλη ετερογενή ομάδα ιών DNA. Κάποιοι από αυτούς τους ιούς έχουν την ικανότητα να προσβάλλουν τον άνθρωπο και να ενσωματωθούν στο ανθρώπινο γενετικό υλικό παραμένοντας εκεί καθ’ όλη τη διάρκεια της ζωής του. Σήμερα, έχουν ταυτοποιηθεί περισσότεροι από 120 τύποι ιών θηλωμάτων που προσβάλλουν τον άνθρωπο (HPV), ενώ διαρκώς ταυτοποιούνται νέοι. Σαράντα (40) από τους 120 ιούς HPV θεωρούνται σεξουαλικώς μεταδιδόμενοι και μεταδίδονται κυρίως με τα υγρά του σώματος κατά τη διάρκεια της σεξουαλικής επαφής.
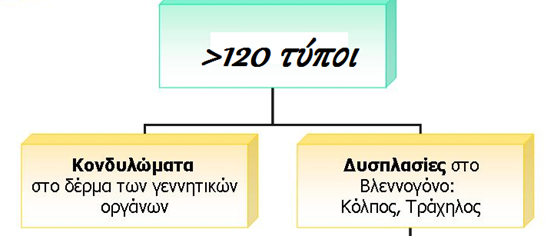
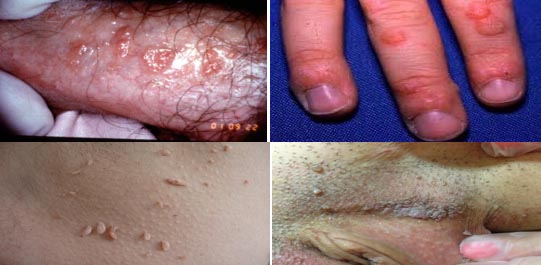
Οι HPV προσβάλλουν το πλακώδες επιθήλιο του δέρματος και των βλεννογόνων, συμπεριλαμβανομένων των βλεννογόνων του στόματος και του φάρυγγα, τον τράχηλο της μήτρας, τον κόλπο και τον πρωκτό. Αυξάνουν τη μιτωτική του δραστηριότητα και προκαλούν την εμφάνιση διαφόρων αλλοιώσεων, η φύση των οποίων εξαρτάται από την περιοχή του σώματος και του τύπου του ιού.
Η HPV μόλυνση
Η μόλυνση του επιθηλίου από τον ιό του ΗPV μπορεί είτε να παραμείνει σε λανθανούσα κατάσταση είτε να εξελιχθεί σε λοίμωξη με την δημιουργία κλινικής ή υποκλινικής νόσου. Είναι πιθανό, κάποια στιγμή η μόλυνση να εξελιχθεί σε υποκλινική φλεγμoνή, η οποία μπορεί να κατασταλεί και να μεταπέσει και πάλι σε λανθάνουσα κατάσταση. Σε έφηβους και νεαρούς ενήλικες, η διαδικασία αυτή είναι συνήθης με αποτέλεσμα η προσβολή από ΗPV να είναι παροδική. Ωστόσο, σήμερα γνωρίζουμε ότι τα άτομα που φέρουν άτυπες μορφές του HPV μεταδίδουν τον ιό στους σεξουαλικούς συντρόφους κανονικά. Συχνά, σε άτομα που έχουν μολυνθεί από τον ιό, δεν είναι ορατή ούτε μακροσκοπική ούτε μικροσκοπική αλλοίωση. Ο χρόνος επώασης της λοιμώξης από τον ΗPV κυμαίνεται συνήθως από 3 εβδομάδες έως 8 μήνες. Πολλές φορές όμως, το χρονικό διάστημα μεταξύ προσβολής από τον ιό και κλινικής εκδήλωσης της νόσου, μπορεί να είναι ως και 10 χρόνια μετά! Επιδημιολογικές μελέτες έχουν δείξει ότι στην πλειοψηφία των περιπτώσεων, μια τυχαία κυτταρική μόλυνση δεν εξελίσσεται απαραίτητα σε φλεγμονή και παραμένει σε λανθανούσα μορφή για μεγάλα χρονικά διαστήματα.
Η HPV φλεγμονή
Η HPV φλεγμονή διακρίνεται σε μη παραγωγική και παραγωγική. Στο στάδιο της μη παραγωγικής φλεγμονής, το γονιδίωμα του ιού ενσωματώνεται με τυχαίο τρόπο στα χρωματοσώματα του ξενιστή. Αντίθετα, στο στάδιο της παραγωγικής φλεγμονής, το γονιδίωμα του ιού αναδιπλασιάζεται ως πλασμίδιο (επίσωμα) ξεχωριστά από το γενετικό υλικό του ξενιστή. Εκ πρώτης όψεως, μπορεί η μη παραγωγική φάση να φαίνεται λιγότερο επιβλαβής όμως, η ενσωμάτωση του HPV στο γονιδίωμα του ανθρώπου, δύναται να τροποποιήσει την εκφράση ιικών πρωτεϊνών και να οδηγήσει σε καρκινογένεση. Συνήθης στόχος του ιού αποτελεί η βασική στιβάδα του επιθηλίου, όπου πραγματοποιούνται οι κυτταρικές διαιρέσεις. Η πρόσβαση των ιών στη στοιβάδα αυτή, εξασφαλίζεται μέσω μικροτραυματισμών του δέρματος, γι’ αυτό και η σεξουαλική επαφή (κολπική, στοματική ή/και πρωκτική) αποτελεί τον κυριότερο τρόπο μετάδοσης του ιού διότι, εξαιτίας της τριβής είναι πολύ εύκολο να δημιουργηθούν επιθηλιακές αμυχές. Σημαντικό ρόλο παίζει ο αριθμός των σεξουαλικών συντρόφων ενώ η πλειονότητα των σεξουαλικά ενεργών γυναικών και ανδρών θεωρείται πως θα μολυνθούν μια φορά στη ζωή τους από
κάποιο υπότυπο ΗPV. Η άμεση δερματική επαφή με τη νοσούσα από HPV περιοχή αποτελεί ένα δευτερεύοντα, αλλά όχι σπάνιο, τρόπο μόλυνσης. Ο ιός είναι δυνατόν να δεισδύει στα επιθηλιακά κύτταρα ενός υγιούς οργανισμού, τόσο μέσω τραυματισμών όσο και μέσω μικρών εκδορών του δέρματος ή του βλεννογόνου, μετά από δερματική επαφή με καποιό μολυσμένο άτομο.
Τυποποίηση HPV
Αναλόγως του τύπου του ΗPV και των βλαβών που προκαλεί οι ιοί χαρακτηρίζονται ως υψηλού κινδύνου, χαμηλού κινδύνου και μέτριου κινδύνου. Η ανάλυση της αλληλουχίας DNA των HPV βοηθάει στην ταυτοποίηση και κατηγοροποίηση τους και τελικά σε μια πρόβλεψη των πιθανών αλλοιώσεων που αναμένεται να εμφανιστούν στον άνθρωπο μετά από μόλυνση με κάποιον από αυτούς τους τύπους. Τα θηλώματα στα γεννητικά όργανα χρειάζεται να διαφοροδιαγνωστούν κάνοντας ταυτοποίηση του τύπου του HPV. Κάποια άτομα φαίνεται ότι είναι πιο ευαίσθητα στο να μολυνθούν HPV σε σχέση με άλλα.
Πρόληψη και έγκαιρη διάγνωση
Οι ήδη υπάρχουσες μεθόδοι για την ανίχνευση των HPV στηρίζονται συνήθως στην ανίχνευση μορφολογικών αλλαγών που έχει ήδη προκαλέσει ο ιός στα επιθηλιακά κύτταρα. Στις μεθόδους αυτές συγκαταλέγονται η κυτταρολογική εξέταση (ΤΕΣΤ ΠΑΠ), η πιο εξελιγμένη μέθοδος της κυτταρολογίας υγρής φάσης (η οποία θέτει και την υποψία της υποκλινικής νόσου) και η κολποσκόπηση κατά την οποία αποκαλύπτονται οι υπάρχουσες αλλοιώσεις.
Με αυτές τις «κλασσικές» μεθόδους, η διάγνωση του HPV γίνεται αφού έχει προηγηθεί η βλάβη ενώ δεν υπάρχει η δυνατότητα ανίχνευσης του ιού σε λανθάνουσα κατάσταση αλλά ούτε και η ανίχνευση προκαρκινικών καταστάσεων. Το ΤΕΣΤ ΠΑΠ δεν δίνει την δυνατότητα λήψης υλικού προς ανάλυση από άλλες περιοχές εκτός από της γεννητικής περιοχής καθώς επίσης παρουσιάζει μειονεκτήματα τόσο στη συλλογή του υλικού όσο και στην επεξεργασία, με αποτέλεσμα συχνά να εμφανίζονται είτε ψευδώς θετικά είτε ψευδώς αρνητικά αποτελέσματα.
Η πρόληψη και η έγκαιρη διάγνωση για HPV είναι δυνατή διενεργώντας συγκεκριμένες αναλύσεις για την ανίχνευση του ιού σε επίπεδο DNA. Οι μόνες μέθοδοι που ανιχνεύουν και τυποποιούν τους ΗPV πριν το στάδιο της παραγωγικής φλεγμονής είναι η ανάλυση της αλληλουχίας του DNA των HPV. Η ταυτοποίηση και κατηγοροποίηση τους μπορεί να βοηθήσει στην πρόβλεψη πιθανών αλλοιώσεων που αναμένεται να εμφανιστούν στον άνθρωπο.
Η καινοτόμος μέθοδος του HPV–DNA Test δίνει τη δυνατότητα της συλλογής δείγματος από διάφορες περιοχές του σώματος εντοπίζοντας έτσι τον ιό σε επιθηλιακούς ιστούς, Η μέθοδος ΗPV-DNA TEST είναι ικανή να ανιχνεύει τον HPV έγκαιρα και με μεγάλη ευαισθησία, καθορίζοντας τον τύπο του ιού πριν προκληθούν μορφολογικές αλλοιώσεις. Η διάγνωση είναι άμεση και ο θεράπων ιατρός μπορεί έγκαιρα να προβεί στην κατάλληλη θεραπευτική αντιμετώπισή του.

