The papilloma virus (Papilomma virus, PV) belongs to a large heterogeneous group of DNA viruses. Some of them viruses have the ability to they offend man and to be incorporated into human genetic material remaining there throughout his life. Today, they have been identified more than 120 types of papillomaviruses that infect humans (HPV), while new ones are constantly being identified. Forty (40) of the 120 HPV viruses are considered sexually transmitted and are mainly transmitted with body fluids during sexual intercourse.
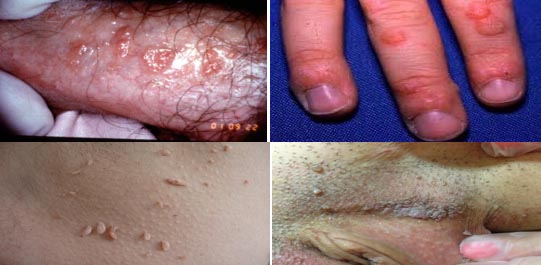
The HPVs offend the squamous skin epithelium and mucous membranes, including the mucous membranes of the mouth and pharynx, cervix, vagina and anus. They increase its mitotic activity and cause the appearance of various lesions, the nature of which depends on the area of the body and the type of virus.
THE HPV contamination
The pollution of the epithelium by the HPV virus it can either remain in a dormant state or to develop into an infection with the creation of clinical or subclinical disease. It is possible that at some point the infection will develop into a subclinical inflammation, which can be suppressed and go into a latent state again. In teenagers and young adults, this process is common and the HPV infection is transient. However, today we know that the people who carry informal forms of it HPV transmit the virus to sexual partners normally. Often, in people infected with the virus, neither macroscopic nor microscopic lesion is visible. THE incubation period of HPV infection usually varies from 3 weeks to 8 months. Many times, however, the time interval between infection by the virus and clinical manifestation of the disease, it can be up to 10 years later! Epidemiological studies have shown that in the majority of cases, a random cellular infection does not necessarily develop into inflammation and remains latent for long periods of time.
THE HPV inflammation
HPV inflammation is divided into non-productive and productive. In the non-productive inflammation stage, the viral genome is randomly integrated into the host's chromosomes. In contrast, in the productive inflammation stage, the viral genome replicates as a plasmid (episome) separate from the host's genetic material. At first glance, the non-productive phase may seem less harmful, but its incorporation HPV in the human genome, may modify the expression of viral proteins and to lead to carcinogenesis. A common target of the virus is the basal layer of the epithelium, where cell divisions take place. The access of the viruses to this layer is ensured through micro-injuries of the skin, which is why sexual contact (vaginal, oral and/or anal) is the main way of transmission of the virus because, due to friction, it is very easy to create epithelial cracks. An important role is played by the number of sexual partners while The majority of sexually active women and men are expected to be infected at least once in their lifetime
some subtype HPV. Direct skin contact with the HPV-afflicted area is a secondary, but not rare, mode of infection. The virus can penetrate the epithelial cells of a healthy organism, both through injuries and through small abrasions of the skin or mucous membrane, after skin contact with an infected person.
Standardization HPV
Depending on the type of HPV and the damage it causes viruses are classified as high risk, low risk and moderate risk. The sequence analysis DNA of HPV helps to identify and categorize them and finally to a prediction of the possible lesions expected to appear in man after infection with one of these types. Genital papillomas need to be differentially diagnosed by identifying the type of HPV. Some people seem to be more susceptible to getting infected with HPV than others.
Prevention and early diagnosis
The already existing methods for the detection of HPV are supported usually in the detection of morphological changes where he's got already cause the virus in epithelial cells. These methods include the cytological examination (PAP TEST), the most advanced method of liquid phase cytology (which also raises the suspicion of subclinical disease) and colposcopy during which the existing lesions are revealed.
With these "classical" methods, his diagnosis HPV occurs after the damage has occurred while there is no possibility of detecting the virus in a latent state, nor the detection of precancerous conditions. The PAP TEST does not allow obtaining material for analysis from areas other than the genital area and also presents disadvantages both in the collection of the material and in the processing, as a result of which either false positive or false negative results often appear.
Prevention and early diagnosis for HPV is possible by conducting specific analyzes to detect the virus at level DNA. The only methods that detect and standardize HPV before the stage of productive inflammation is the analysis of the HPV DNA sequence. Their identification and categorization can help in prediction of possible alterations expected to occur in humans.
His innovative method HPV–DNA Test enables her collection of samples from different areas of the body thus locating the virus in epithelial tissues, The HPV-DNA TEST method is capable of detecting HPV timely and with great sensitivity, determining the type of virus before morphological changes occur. The diagnosis is immediate and the attending physician can promptly proceed with the appropriate therapeutic treatment.

